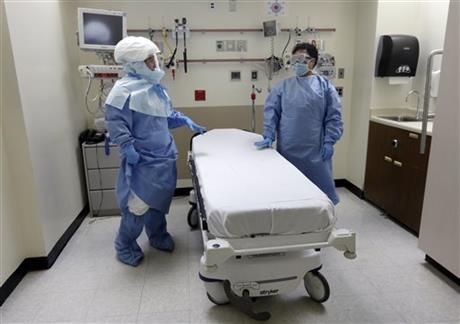
The Associated Press

The U.S. health care apparatus is so unprepared and short on resources to deal with the deadly Ebola virus that even small clusters of cases could overwhelm parts of the system, according to an Associated Press review of readiness at hospitals and other components of the emergency medical network.
Experts broadly agree that a widespread outbreak across the country is extremely unlikely, but they also concur that it is impossible to predict with certainty, since previous Ebola epidemics have been confined to remote areas of Africa. And Ebola is not the only possible danger that causes concern; experts say other deadly infectious diseases — ranging from airborne viruses such as SARS, to an unforeseen new strain of the flu, to more exotic plagues like Lassa fever — could crash the health care system.
To assess America’s ability to deal with a major outbreak, the AP examined multiple indicators of readiness: training, manpower, funding, emergency room shortcomings, supplies, infection control and protection for health care workers. AP reporters also interviewed dozens of top experts in those fields.
The results were worrisome. Supplies, training and funds are all limited. And there are concerns about whether health care workers would refuse to treat Ebola victims.
Dr. Jeffrey S. Duchin, chairman of the Public Health Committee of the Infectious Diseases Society of America and a professor of medicine at the University of Washington, said it will take time to ramp up readiness, including ordering the right protective equipment and training workers to use it. “Not every facility is going to be able to obtain the same level of readiness,” he said.
AP reporters frequently heard assessments that generally, the smaller the facility, the less prepared, less funded, less staffed and less trained it is to fight Ebola and other deadly infectious diseases.
“The place I worry is: Are most small hospitals adequately prepared?” said Dr. Ashish Jha, a Harvard University specialist in health care quality and safety. “It clearly depends on the hospital.”
He said better staff training is the most important element of preparation for any U.S. Ebola outbreak. He believes a small group of personnel at each hospital needs to know the best procedures, because sick people are likely to appear first at medium-size or small medical centers, which are much more common than big ones.
Jha pointed to stepped-up training in recent weeks but wondered, “Will it be enough? We’ll find out.”
A high ranking official at the U.S. Department of Health and Human Services said Wednesday that the government does not expect every hospital in America to be able to treat an Ebola patient, but “every hospital has to be able to recognize, isolate and use the highest level of personal protective equipment until they can transfer that patient.”
“The moment anyone has an Ebola patient, (the U.S. Centers for Disease Control and Prevention) will have a team on the ground within a matter of hours to help that hospital,” Dr. Nicole Lurie, the HHS assistant secretary for preparedness and response, said Wednesday. She acknowledged “some spot shortages of personal protective equipment” but said many kinds “‘are still pretty widely available” and that manufacturers are ramping up production.
___
AN OVERTAXED EMERGENCY CARE SYSTEM
Without any stress caused by Ebola cases, the emergency care system in the U.S. is already overextended. In its 2014 national report card, the American College of Emergency Physicians gives the country a D-plus grade in emergency care, asserting the system is in “near-crisis,” overwhelmed even by the usual demands of care.
In a CDC study on hospital preparedness for emergency response in 2008, the latest data available, at least a third of hospitals had to divert ambulances because their emergency rooms were at capacity.
Add an influx of people with Ebola, along with those who fear they might have the disease, and the most vulnerable segments of the health care system could wobble.
“Even though there have been only a couple cases, many health systems are already overwhelmed,” said Dr. Kenrad Nelson, a professor at Johns Hopkins Bloomberg School of Public Health and former president of the American Epidemiological Society, referring to new federal procedures for screening, tracking and treating the disease and people who are exposed. He added that if a major flu outbreak also occurred, “it would be really tough.”
“We’re really going to have to step up our game if we are going to deal with hemorrhagic fevers in this country,” said Lawrence Gostin, a global health law expert and professor at Georgetown University.
How big of an outbreak would it take to overpower the U.S. health care system?
“It would have to be only a mediocre outbreak,” said Gostin. “The hospitals will be flooded with the ‘worried-well.’ People with influenza or other infections that are not Ebola could jam up the public health system.”
One federal study on emergency room visits indicated that at least 4 percent of visits involved patients with fever — a common symptom of Ebola. Combining fevers with stomach pain, headaches and coughs, about a fifth of emergency visits involve symptoms often seen in Ebola patients.
A doctor who had recently treated Ebola patients in West Africa came into Bellevue Hospital in New York City last week with a fever and gastrointestinal symptoms. In announcing the man had been placed in isolation, officials pointed out how his symptoms also could be consistent with salmonella, malaria or the stomach flu.
Last Thursday, the doctor tested positive for Ebola.
___
UNEVEN LEVEL OF PREPAREDNESS
National surveys have repeatedly found that while most health care providers are willing to care for people with dangerous diseases like Ebola, they generally feel unprepared to do so.
Personnel at almost all hospitals in the Black Book survey said their facilities were not capable of quarantining large numbers of people possibly exposed to Ebola.
Nearly three-quarters of emergency doctors and four in five infection specialists at large hospitals felt their facilities were not adequately prepared to deal with Ebola patients.
Hospital administrators and medical staff had widely divergent perspectives on their facilities’ ability to treat the disease. Among medical staff at big hospitals, nearly all who participated in the survey believed their hospitals were not adequately staffed and trained for Ebola patients. About two in three of administrative and financial staff shared that worry.
Among emergency nurses, nearly all worried about the impact of emergency department crowding on the ability to deal with Ebola patients; just more than half of administrative and financial managers felt that way.
Other striking results: Personnel at only 1 percent of surveyed acute care hospitals said they can handle more than 10 Ebola patients at once. That was true at just about one-quarter of academic medical centers.
A demonstrated weakness of U.S. hospitals in controlling other hospital-acquired infections also suggests a soft spot in Ebola readiness. In 2011, the most recent year of data, about 75,000 hospital patients with health care-associated infections died during their hospitalizations, according to a national CDC survey published this year. Such infections are considered to be a proxy to measure hospitals’ readiness to contain Ebola.
Added Douglas Brown, managing partner at Black Book: “We got a lot of feedback that community hospitals aren’t the place for Ebola patients to come.”
___
SUPPLY SHORTAGES AND SURGE WORRIES
Shortages abound, beginning with the fact there are only four specialized containment care facilities set up to isolate and treat patients with Ebola and other very dangerous diseases. In any sizable outbreak, those dozen or so beds would fill up very quickly.
Appropriate equipment could be in short supply for mid-size and smaller hospitals, and even some larger ones. CDC estimates from 2008, the most recent available national figures, put the average number of protective suits with powered air-purifying respirators per hospital at 10. The average hospital had six mechanical ventilators, which could be needed for Ebola patients with breathing problems.
A recent nationwide survey of state public health departments suggests not all are ready to ramp up quickly. The 2013 National Health Security Preparedness Index, carried out by CDC in partnership with the Association for State and Territorial Health Officials, ranks state health departments on a scale of 1 to 10 on numerous emergency measures. In the category of “surge management,” the average score was 5.8.
Dr. Amesh Adalja, a member of the Public Health Committee of the Infectious Disease Society of America, says some emergency departments are so consumed by the typical number of patients that a surge of any kind can overwhelm them. With an Ebola outbreak, he said, “they’re not just getting a surge of patients, they’re getting a surge of patients with special needs.”
The AP review found evidence that the federal emergency public health network, which is designed to step in to prevent shortages of medicine and medical supplies while local response capacity ramps up, is failing to perform as planned.
Since 2007, Ebola has been identified as a potential threat requiring priority attention under the Public Health Emergency Medical Countermeasures Enterprise, which coordinates the development, stockpiling and dispensing of drugs during a massive disease outbreak or to protect against chemical, biological, radiological or nuclear agents.
The National Institute of Allergy and Infectious Diseases has spent nearly $500 million on Ebola research since 2003. At least another $269 million has been spent on Ebola research under a Defense Department chemical and biological defense program. Some of that funding was spent on vaccine research and better diagnostic testing.
But in October 2011, the Government Accountability Office reported that an anticipated budget for drug acquisitions still had not been produced. Without clear guidance about government funding, pharmaceutical and other medical companies might not want to invest millions of dollars to develop vaccines that are less lucrative than other drugs they could make, the report underscored.
The GAO issued another critical report in December 2013, faulting the program for its “almost 10-year efforts and the continuing lack of available countermeasures.”
None of that stopped a top federal preparedness official from telling Congress in February that the program is “a model for innovative governance and accountable decision-making.”
In fact, the feds’ Biomedical Advanced Research and Development Authority did not fund its first investment in an experimental Ebola treatment until this year because that program only supports potential treatments in a later phase of development. HHS said a relatively modest $25 million has gone to study ZMapp, an experimental drug in short supply that has been provided to numerous infected Ebola patients. Lurie acknowledged Wednesday that funding limitations had contributed to some of the delay in vaccine development.
Given that there is no Ebola vaccine, the government does not have a stockpile of disease-specific drugs on hand, as it has had for pandemic flu.
Also, as of last week, there were no national emergency stockpiles of the waterproof gowns, surgical hoods, full face shields, boot covers or other gear that the CDC recommends for treating Ebola patients. CDC’s $6.2 billion Strategic National Stockpile had just a small quantity of older model gowns on hand, since most were sent to the states during the 2009 swine flu pandemic and had not been replenished, said Greg Burel, director of the agency’s stockpile division. Last Thursday, the agency placed an order to purchase a limited amount of Ebola-specific personal protective equipment, but Burel would not say how much was ordered, or when the goods would be available for distribution.
If the U.S. sustains a major Ebola outbreak, the mechanism for confirming individual patient test results also could be quickly overwhelmed, though the testing situation suddenly is improving. For years, spending on diagnostic research has lagged under the National Institute of Allergy and Infectious Diseases and a Defense Department chemical and biological defense program. The CDC noted in August that the agency and the military had “the only U.S. laboratories capable of conducting diagnostic testing to confirm that a patient has Ebola and not some other illness.” As of Friday, though, the CDC said there were 23 additional labs that have the expanded diagnostic technology, primarily local and state health departments.
___
WORRIES ABOUT TRAINING
Shortcomings in training and preparedness for health care workers are pronounced, and chronic.
More than half of working registered nurses reported they neither received nor provided emergency training during the previous year, according to a study HHS published in 2010 using 2008 data. Of those registered nurses who did receive or provide emergency training, 44 percent felt somewhat or not at all prepared.
Regarding epidemic response planning, a third of hospitals had no plans for alternate care areas with beds, staffing and equipment, according to a study published in 2011 by CDC’s National Center for Health Statistics, again based on 2008 data. Only half had priority-setting plans to get the most use from a limited supply of ventilators. More than a third had no plans for on-site, large-capacity morgues, and a third had no plans for staff absences as a result of the personal or family impact of any epidemic.
A recent survey of 2,500 members of the local health officials’ association found that only one in three local health departments had participated in full-scale emergency preparedness exercises or drills.
Gostin, the global health law expert from Georgetown, thinks the contamination of two nurses at Texas Health Presbyterian hospital in Dallas, where the first person diagnosed with Ebola in the U.S. died, “was not an anomaly.”
He said the U.S. may have the most advanced health care system in the world, but the system is very fragmented because “there’s no uniform national quality control.”
There is great inconsistency in the frequency of emergency drills. According to the Black Book report, only a quarter of academic medical centers had epidemic or biological warfare drills in the previous year, but just 4 percent of medium-size hospitals ran such exercises, and no small hospitals did.
Kristi L. Koenig, director of the Center for Disaster Medical Sciences at the University of California-Irvine, said every hospital needs to have some basic level of preparation, in order to manage the initial treatment. But she suggested the best solution is to increase the number of specialized biocontainment centers.
Such centers would help keep workers safe and properly prepared, not just for Ebola but also for other very dangerous diseases like SARS — severe acute respiratory syndrome — or influenza.
Dr. Phil Smith, who heads the biocontainment unit at Nebraska Medical Center, said that staffers in the typical hospital isolation ward have had little or no practice in putting on and taking off safety gear, or following other procedures for handling Ebola patients. Such practices are second nature at field hospitals and clinics operating in Africa, and are drilled regularly at specialized containment facilities in the U.S.
___
FEARS OF ABANDONMENT
Like nuclear radiation, the Ebola virus, which causes massive internal bleeding and organ failure, touches on deep human fears of a fatal invisible menace. Those fears are shared not only by patients, but also by some professionals who treat them.
In the Black Book Ebola readiness survey released in August, some medical staff said they believed they would stay away from work to shun Ebola patients admitted to their hospitals.
Among isolation care doctors and nurses, 14 percent said they’d call in sick, and one in four critical care and emergency staff said the same. Among the isolation care staff, 17 percent said they wouldn’t work near Ebola patients; half of critical care and emergency staff said the same.
“I think that’s a very valid concern,” said Dr. Melinda Moore, a scientist at Pardee RAND graduate school who has worked as a global health expert for the CDC. “It’s been described in literature and studies.”
She said training on safe Ebola treatment and education for health care workers is the antidote.
Adalja, a member of the Public Health Committee of the Infectious Disease Society of America, called the survey findings troubling and contended they show that many medical staffers “are not confident in the infection control procedures at their hospital.”
Dr. Kenneth Anderson, who leads the research and education affiliate of the American Hospital Association, confidently pointed to the professionalism of most health care workers in the AIDS, H1N1 flu and other past American epidemics as an indication “our staff will step up.”
But Nelson, of Johns Hopkins, pointed to the “huge problem” in Africa, where health care workers have walked off the job. “I think that could be a problem in the United States, because a lot of the population is really terrified,” he said.
___
AP national investigative reporters Holbrook Mohr in Jackson, Mississippi; Michael Kunzelman in Baton Rouge, Louisiana; and David B. Caruso in New York contributed to this story.