It seems we can’t find what you’re looking for. Perhaps searching can help.
Nothing found
Latest Articles
-
 By Jackie Hampton, Publisher, Jackson native Zeita Merchant is the current Commanding Officer of the U.S. Coast Guard Personnel Service Center. She is the first female African American to be appointed rear admiral lower half [...]
By Jackie Hampton, Publisher, Jackson native Zeita Merchant is the current Commanding Officer of the U.S. Coast Guard Personnel Service Center. She is the first female African American to be appointed rear admiral lower half [...] -

-

-

-

Popular Articles
-
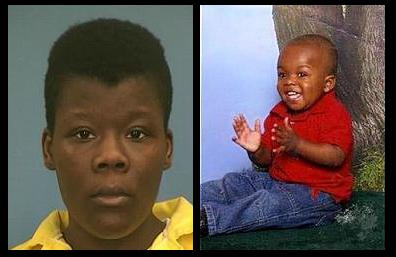 By Monica Land GREENVILLE – A 25-year old woman has been sentenced to life in prison after she admitted she put her son in the oven while he was still alive. Terri Robinson appeared in [...]
By Monica Land GREENVILLE – A 25-year old woman has been sentenced to life in prison after she admitted she put her son in the oven while he was still alive. Terri Robinson appeared in [...] -

-

-

-

